Symptoms to Diagnosis
When I turned 36 I decided I wanted to run a marathon by the time I was 40. It felt important to accomplish something so intensely physical before I got “old”. So I got new running shoes and began the long journey of moving from 0 to 26.2. I will never fully understand why I chose this goal as I have never been a runner. In fact, I have always hated running. My brother is an elite runner, not me.

The first few times I went out I noticed that my right leg seemed to just stop working after not very long. It became hard to pick up my foot and the whole leg just bonked out long before the other. Simultaneously started to notice a twinging, electrical pulsing down the back of my left leg. Did I go and see my doctor? Of course not, why would I do that when a chiropractor could be so much more helpful? I was sure it was just some sort of nerve pinch or alignment issue so I spent close to a year seeing a chiropractor. Nothing was resolving and he finally recommended I see a neurologist.
In October 2007 I had my first of what would become never-ending neurology appointments. She tested my hands and my feet and my reflexes. She reviewed my medical history. She determined that what I was experiencing was not a peripheral nervous system issue (nerve pinch or alignment issue). Instead I was dealing with something in my central nervous system, and she referred me for an MRI. There were keywords from that appointment that Nils and I immediately went home and googled. By the time the evening was over, I felt pretty clear I was looking at multiple sclerosis and praying that I wasn’t looking at ALS.
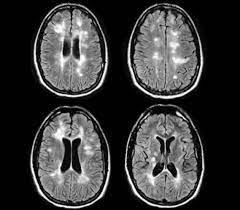
The MRI came back with conclusive evidence of classic multiple sclerosis. Deep breath. What the heck does this mean? For the most part I felt “normal”, not different than I was before and not different than anyone else. It was an abstract and frightening new reality.
I was 37 and definitely not going to be running a marathon.
The Early Years
Management of my MS began that day. The first step was to name the specific flavor of the disease, in my case Relapsing Remitting Multiple Sclerosis (RRMS). This is the form of multiple sclerosis where you have a baseline physical profile, which for me was mostly perfectly fine with “foot drop” and some peripheral neuropathy (numbness) in my hands and feet. With RRMS you will have “relapses” or “flares” where something happens, such as: temporary blindness, temporary full or partial body paralysis, or the sensation of spiders crawling all over half your body – to name a few. These flares could last hours, days, weeks, or months, then things return back to baseline. Mind you, I didn’t have any of those flares I described, those are just some of the more common ones. Approximately 80% of people diagnosed with multiple sclerosis are classified as RRMS at the beginning.
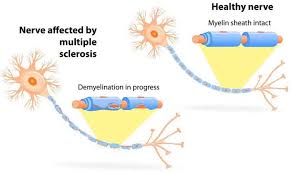
A relapse or flare is connected to a new “lesion” in the brain, a place where your body’s immune system has attacked the myelin sheath of a nerve causing an inflammatory hotspot and breaking down the connection and signal of that nerve to whatever it was supposed to do. The initial inflammation caused by this “attack” usually recedes, often with high dose steroids, but the underlying nerve damage does not heal. That nerve damage does not always cause lasting external symptoms.
Medical management of multiple sclerosis, when one has the relapsing remitting flavor, involves a “disease modifying therapy” or DMT medication. When I was diagnosed in 2007, there were only a handful of options. Today, there are many more choices for people with RRMS and very few (namely one) for individuals with primary or secondary progressive multiple sclerosis, but more on that later.
My neurologist said she wanted me to start on a medication called Rebif, a beta interferon class of medication that involved a self-administered, subcutaneous injection three times per week. I was awarded my very own home healthcare nurse who came out to teach me how to administer the medication and she brought along with her the very encouraging information that she believed multiple sclerosis would be cured within 10 years. Note to any and all medical practitioners, don’t do that.
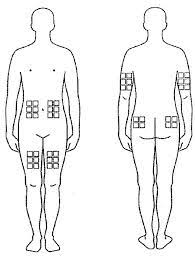
I started giving myself shots every three days in alternating locations that included my abdomen, my thighs, and my butt. You have to rotate because your skin isn’t very tolerate of the medication and “injection site reactions” of redness, swelling, and mild pain make it necessary to spread the dermal trauma around your body.
I don’t remember clearly how long this lasted, but somewhere during that first year I began to feel run down and frequently nauseous. A blood draw revealed that my liver was very insulted by this medication. It was determined that I could not tolerate the beta interferon class of medications which, at the time, ruled out most of the options.
The Middle Years
The next collection of years is blurry in my memory. The first year went by with my original neurologist at the end of which I had another set of MRI tests that determined nothing had changed, meaning there were no new lesions and no visible inflammatory markers in my brain or spinal cord. At that point, she classified me as primary progressive multiple sclerosis (PPMS) and said there was nothing more she had to offer me. She would see me in a year.
Different from RRMS, PPMS at that time had no DMT options. I was set adrift with this dark cloud of diagnosis and no clear action steps available to me. My personality does not sit well not taking action and I decided to switch neurologists.
I researched and found a hotshot neurologist at Virginia Mason Medical Center in Seattle. I immediately loved her. She was smart, she was young, she was direct and scientific. The first thing she said to me was that she didn’t subscribe to providing care based on the different classifications of multiple sclerosis that she said were research, not clinically derived. She would work to see what, if any, treatment might benefit me.
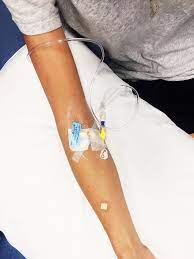
We reviewed options and decided that I would try medication called Tysabri. This medication is complicated. It is a once-a-month infusion instead of self-administered injections and it runs a pretty serious risk of developing what is called PML (progressive multifocal leukoencephalopathy), “a rare and usually fatal viral disease that is characterized by progressive damage or inflammation of the white matter of the brain.” Basically, it is like mad cow disease. It is only a risk if you have a very specific virus known as the “JC” virus. This virus is super common and for the most part no one even notices they have it. However, when you go on an immunosuppressive medication, the virus can take hold and cause PML.
It is a very serious decision to take Tysabri and at the time I started there was no test for the JC virus. However, research showed that during the first year taking Tysabri the risk was low. Starting with the second year, the risk went up exponentially. Another piece I needed to consider is that the once-a-month infusions requires carving out a full day. There’s travel to the appointment, four hours of infusion, observation for reaction, and travel home. No small deal, especially when working full time.
I took Tysabri for a year. As that year ended I had to assess next steps. All DMT medications are immunosuppressive on some level, increasing risk of sickness and infection. There was no change either positive or negative in how my body felt, no change again on my MRI, and the risks of continuing were increasing. I was able to determine that I was JC virus negative which made it safer to stay on Tysabri, but I decided to stop because I felt the risks of immunosuppression weren’t worth the non-discernible benefits. I am guessing we are now at around 2009.
At around this time I switched gears in my life. I decided I wanted to go back to school to get a graduate degree in nutrition. I felt strongly that nutrition was a powerful medicine to support health and healing and I wanted to be a part of it. I spent a year doing healthcare pre-requisite courses needed to apply to the program I wanted to attend. I closed my business as a professional photographer. I also stopped doing any DMT medications because I didn’t feel confident any of them would make a difference and the side effects and risks felt too high.
It is a crazy mind game when you have a progressive form of multiple sclerosis. Almost every DMT is aimed at decreasing or halting the number of flares/exacerbations a person has in a given time span (usually a year interval) documented by MRI changes. If you aren’t having anything that is overtly identifiable on an MRI or experientially documentable with your symptoms, whether or not the medication is working is entirely a leap of faith.

You have no way to know how different your trajectory would’ve been if you hadn’t been on the medication. All DMT medications have side effects and risks. Without the concrete knowledge that they are making a difference, are the risks worth it? Leap of faith.
I focused on life. Being a mom, being a wife, being a student, being a community member, walking, hiking, living. And life was good. In September 2010 I started my graduate program in nutrition science at BASTYR University and I graduated in June 2012. I started my dietetic internship in September 2012 through June 2013. All of this was challenging, stressful, exciting, and ultimately very successful. At the end of it, I was a registered dietitian nutritionist (RDN). My MS was stable throughout this whole time. I learned to ride a motorcycle, I backpacked, I hiked, I exercised, and I generally felt normal. I couldn’t run, but I didn’t really miss it.

Somewhere in there I switched neurologists to a practitioner at the University of Washington Multiple Sclerosis Center. We both agreed that I had a progressive form of MS and there wasn’t an existing DMT that would benefit me. I was in stasis, a holding pattern. I saw physical therapists for my walking and foot drop issues. I saw occupational therapists to help my arm and hand function. Fun fact, physical therapists work on legs and occupational therapist on arms and hands. I would’ve thought that physical therapist did the whole body, but I would be wrong.
After becoming an RDN, I started working as a dietitian at Seattle Cancer Care Alliance (SCCA) in hematopoietic stem cell transplant (HSCT) for patients with leukemia and lymphoma. This will become very relevant later in my story. I also started working in private practice.
Transitioning Ability
In September 2015 I was hired by an exciting startup, Arivale, and I left my private practice and SCCA to take on this more-than-full-time, exciting adventure.

The job involved commuting back and forth to Seattle daily, two hours each way. It involved a very steep learning curve and while all of this was extremely exciting, it was a big stressor on my body. At the same time, I started going through perimenopause.
It’s hard to know how much each of these factors impacted the trajectory of my MS, but my body and symptoms started changing a lot during this time. Over the next few years, I went from walking fast for miles to using a mobility scooter to get from my car to the ferry to my office. I went from being able to handwrite and type to needing voice dictation. I went from having tons of energy to being hit frequently by waves of debilitating fatigue. Stress, both physical and emotional/cognitive, is known to exacerbate symptoms in MS. Perimenopause/menopause is also aknown, though much less studied, contributor to MS progression.
Also during this time my husband, Nils, went through a year-long cycle of cancer treatment and my mother-in-law, who had been living with us for the last 10 years, became very ill and passed away. More stress and intensity.
In 2017 the FDA approved the drug Ocrevus for both relapsing remitting and primary progressive multiple sclerosis.
This was the first DMT ever approved for PPMS. Ocrevus is a “humanized monoclonal antibody” that targets mature B-cells. It is an infusion that you get every six months, and it is approximately $45,000 per infusion. Thankfully, this is covered by insurance if you have it.
I was excited at this opportunity because of how fast my body and life were changing. I took Ocrevus for two cycles (one year) without any noticeable change in progression trajectory or any improvement in symptoms. As I described before, it is impossible to know what would’ve happened had I not taken it and Ocrevus increases your risk of respiratory infection through immunosuppression. I was staring again at the leap of faith cost versus benefits conundrum. I chose to discontinue after one year. Another fun fact, Ocrevus is expected to slow progression for approximately 25% of patients. Not the best odds anyway.
In November 2017, after Nils stabilized out of his cancer treatment, I took two months of medical leave which I had originally intended to take right before he was diagnosed but put on hold to focus on his care.

I returned to work in January 2018 at 75% time (30 hours per week). I was incredibly lucky to have had long-term disability insurance which kicked into gear at this time and covered a percentage of my decreased hours. I was also incredibly lucky that my company was willing to be as accommodating as I needed. At first, I came into the office two days per week and worked from home the rest of the time. I was able to rest when I needed and had a full day off every week. Eventually I needed to work all of my hours from home, which was accommodated.
April 24, 2019 we were called into an “all hands” meeting at work and told the company was officially closing and we needed to be out of the office by noon. Complete shock and surprise. Again, I thankfully was covered by the long-term disability insurance plan I had initiated. If I had not opened my claim prior to the closing of the company, I would’ve been completely screwed. As it stands, I will be receiving income from that LTD plan until I turn 65. I encourage everyone who has access to LTD insurance through their employer to take advantage of it.
I had been contemplating going down to 20 hours per week at work before the company closed. I had been sticking it out to maintain our health insurance coverage which would go away if I dropped below 30 hours per week. Nils was still recovering from cancer treatment and out on disability from a work injury. So, when the company closed, we were flung into scramble mode. My health insurance coverage held through the end of May and then we had to figure out the exchanges for private coverage. My need to rest once again went on the back burner.
Like many of my fellow colleagues, I jumped into high gear to reopen my private practice. I got a new business license, contacted my Arivale clients, started the process of insurance credentialing, began website building and dove into continuing education to build my skills around eating disorders and relationship to food/IntuitiveEating work.
I still had multiple sclerosis. I still had crippling fatigue and very impacting mobility challenges. I still needed to rest.
Leaving The Work World
Sense of purpose and personal identity is a big part of navigating a progressive chronic disease. What does it mean to be a contributing member of your community, your family, the world when your body doesn’t work? So much of my day is navigating my body challenges which crowds out most other pursuits. My drive to keep working was, in large part, my need/want to hold on to that professional identity, to have an answer to the social question, “So, what do you do?”. But to do that, I was pushing hard, too hard. Building a business is a scramble that takes a lot of energy. Energy I didn’t really have.
The rest of 2019 and all of 2020 (adding on the stress of the first year of Covid) I gave it a go. I kept a small handful of clients but I didn’t push to find more. I didn’t have it in me.
Near the end of 2020 the long-term disability company reached a benchmark date in the timeline of my case where it determined I needed to apply for Social Security disability income (SSDI). This ended up making the decision for me of whether or not I would keep working.

Applying for SSDI is a very confronting process where you must prove, in intricate detail, how broken and nonfunctional your body is. You must detail exactly how you can’t really do anything to contribute to “meaningful work”. You have to fight to convince others how hard your life is. This is entirely contrary to the need to remain positive and optimistic to have the motivation to do all you can to maintain what you have and feel hopeful.
My New “Job”
In January 2021, I officially stopped working, professionally that is. My work became my wellness, and that can be a really confusing thing. What does it mean to be well when you can’t heal what’s breaking your body apart?
Throughout my 15 years of living with multiple sclerosis I have tried many different nutrition regimens intended to fortify my body, decrease inflammation, regenerate nerves, stop disease progression, repair damage, etc. Swank Diet, Whal’s Protocol, Mediterranean Diet, Anti-Inflammatory Diet. If you recall, I got a graduate degree in nutrition science specifically to see what I could do to heal from chronic disease. But multiple sclerosis is not a nutritional disease. It is a disease of the immune system gone awry. I have come to recognize that I can provide my body with the tools to support its optimal function, and that’s a good thing to do, but I’m not going to have a miracle recovery by eating kale and nutritional yeast.
Over the years I have seen a dozen different physical therapists. I’ve seen a small handful of occupational therapists. I’ve tried aqua therapy, chiropractic care, acupuncture (multiple different practitioners) Botox injections to decrease spasticity in my arm and hand, and countless braces and “durable medical equipment” devices aimed at improving the function of my leg and arm. The collection of therapeutic apparatus I have accumulated over the last 15 years is almost comical.

As 2021 began and my professional work ended, I committed full time to the most effective pieces of what I’d found in my searching. The first building block is a focused and intentional mindfulness meditation practice to decrease stress and allow my body to live more of the time in the parasympathetic mode. I found an online multiple sclerosis physical therapy program with an evidence-based neuroplasticity foundation, “The MS Gym”. This program became my daily practice, along with in-person physical therapy. Between meditation, stretching, MS gym, physical therapy, and resting, along with all the necessary activities of daily living and managing life and household, this is the basic frame and flavor of my daily life.
Sometime during the summer, I got approved for SSDI which was both a relief to finally have that done and a definition I now got to attach and integrate into myself.
The Road to HSCT
As I mentioned a while back, when I first graduated with my RDN credential, I started working at Seattle Cancer Care Alliance (SCCA) on the HSCT team. The patients I worked with had some form of leukemia or lymphoma – blood-based cancers. They were given medication to stimulate their bone marrow to overproduce hematopoietic stem cells which would be harvested from their blood and stored. Then they would undergo a very rough chemotherapy treatment to obliterate their peripheral and bone marrow immune systems then they would have their stem cells reintroduced in an attempt to rebuild an entirely new immune system free from cancer. This was a months long process that was brutal and risky, but their only chance at saving their life.
At one point I spent a week working on the inpatient side at the University of Washington Medical Center learning the process of patients who had to be admitted for complications. Normally patients did their treatments in an outpatient clinic setting and stayed in an apartment nearby, but sometimes they got a risky infection and needed to be admitted.
During that week, while sitting at a table during rounds, I learned of a patient who had undergone HSCT for multiple sclerosis as part of a trial through the Fred Hutchinson Cancer Research Center. I made a mental note at that time but couldn’t imagine why anyone would do that to their body if MS was the underlying disease. At that time my symptoms were mild to nonexistent.
In the years between then and now I periodically brought up the idea of HSCT to my neurologist, curious to hear her thoughts. She was somewhat dismissive and was glad that I had a first-hand experience of what it meant to undergo that treatment. The research was very young, the benefits not clear, and the risks quite high.
In the fall of 2021, I happened to hear a podcast that talked about two individuals who had undergone HSCT for MS, one in Russia and one in Mexico.
This was really the first time I had actively reconsidered HSCT. It opened my eyes to how many people were undergoing treatment to halt the progression of their MS all over the world. I go into detail about exactly what HSCT is, the protocol, the different types, why I’m choosing to go to Mexico, and what recovery looks like on a separate page.
After hearing that podcast, I dove deeply into research. I listened to more podcasts, I reviewed over 30 research articles with all of the pros and cons, I watched YouTube videos of MS conference presentations, I got involved in Facebook groups and read many patient stories, I had long phone calls with people, both in the US and Canada, who had gone through the process, I asked tons of questions, and I came to the decision that this was the right thing to do, and now was the time. Once I had made the decision, waiting seemed irresponsible. I chose Mexico over Russia and sent in my application. I was accepted into their January 31, 2022 cohort and I started the busy process of getting all my ducks in a row to get onto that plane and head to Puebla, Mexico.

The blog picks up my story from here. Thank you for reading.