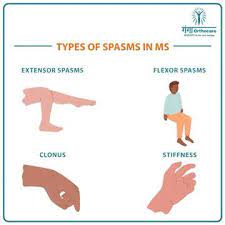
Got Spasticity?
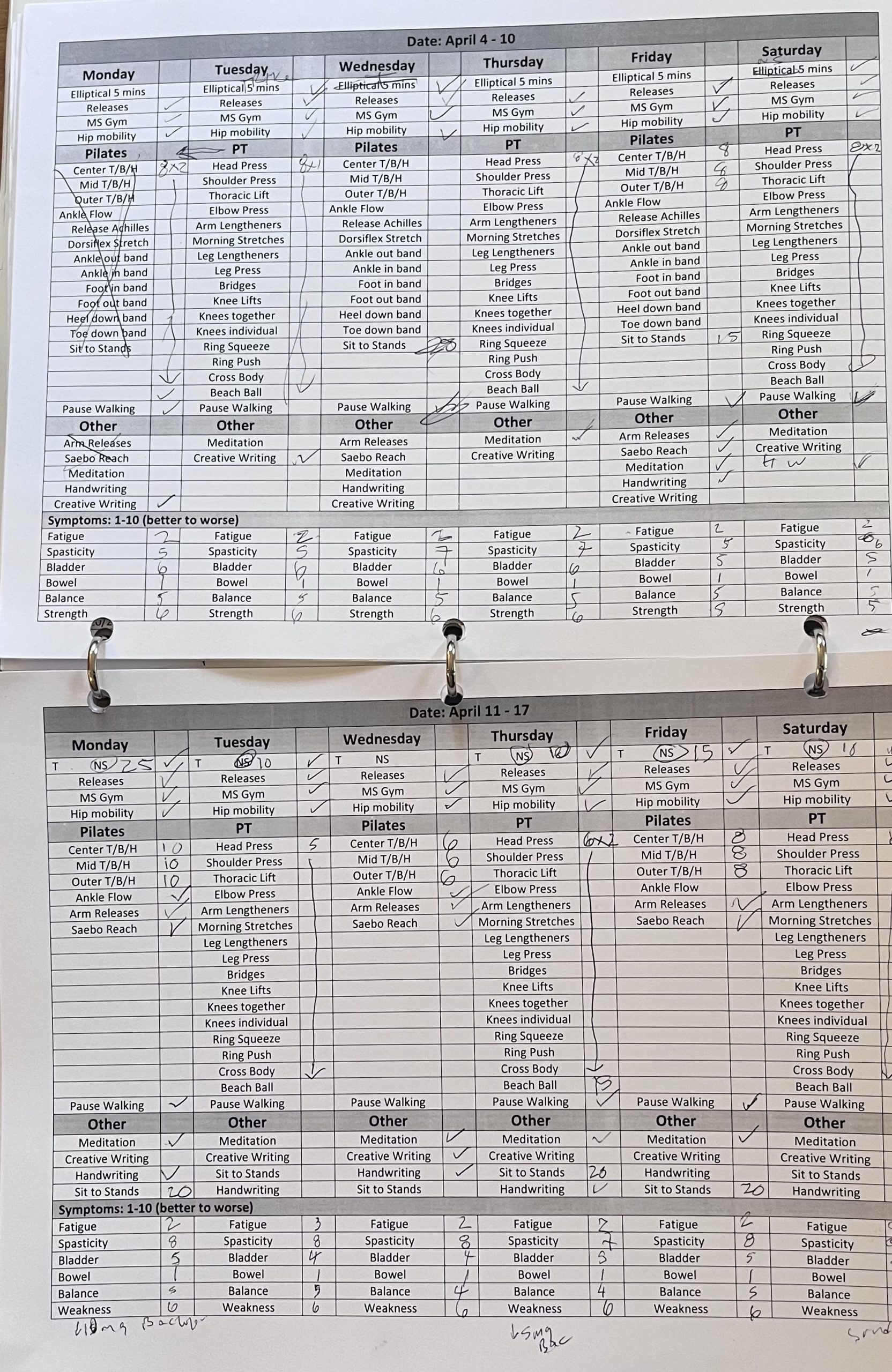
This is the post where I document, on mostly a monthly basis, the experience/progress/reality of my symptoms; tracking how things are moving. I resisted writing this post because I find myself in the long tunnel of recovery. This is the place where things get worse before they (hopefully) get better. I would like to able to report linear progress and tangible outcomes. That’s not how this works
I knew going into treatment that the first year was likely going to be rough. I knew that many people encountered significant increased spasticity. I knew the beast was coming. This beast doesn’t move through quickly. It doesn’t sit down and rest quietly by the hearth. This beast is vigilant, relentless, and resistant, impervious to the slings and arrows of my outrageous fortune. So, I do the best I can. I search out tools and tricks to settle the beast down, to distract it, to make it sleepy, if even momentarily.
My sorceress bag includes gabapentin, baclofen, tizanidine, pot, physical therapy, acupuncture, the swimming pool, zero gravity bed positions, pure wave massagers, tiger tail rollers, therapeutic massage, mindfulness meditation, magnesium glycinate, pelvic floor therapy, vibration plates, lion’s mane mushrooms, Valium, Tramadol, sheer force of will.
Medical Experimentation:

Over the last two weeks I have started gabapentin and titrated up to a current dose of 900 mg three times per day. I started at 300 mg three times a day and thought, “hmmm, I feel something. A tickle of relief.” But it wasn’t enough, and I slowly increased to 600 mg three times a day. At first it felt miraculous. It wasn’t perfect, but I could move more fluidly, more freely, I could feel my legs – they belonged to me. But it was fleeting and inconsistent. I read research that reported the sweet spot dosage of 900 mg three times a day. So that’s where I am now. If I want to, I can go as high as 3600 mg (1200mg 3x or 900mg 4x) per day. I will hang at this dose for a while to see if it settles in and evens out. It seems to not work very well in the morning, only coming online mid to early afternoon. I find I feel best in the evening before bed and the worst in the morning getting out of bed.
Research also shows that it can take up to four weeks for the full impact of the medication to take effect, so I will be patient. If I find it gives me relief more often than not, I will begin to wean off the baclofen, carefully this time, and see if I need to be on both.
I am also doing a more scientific, patient way the use of the different RSO (cannibis oil) strains I have found to be valuable. Here is a little of what I’ve learned:
Milky Way RSO: seems to give some relief but also makes me weirdly high, uncomfortably so. It is not a good high, but a paranoid disconnected one. I don’t understand why because it has very little THC. I want this one to work for me because it has a high CBG content and that is supposed to positively impact many different areas. So far, I kinda hate it but I haven’t quite given up yet.
Sour tsunami RSO: this one does not make me feel high until I take a very high dose. Its THC content is the same as Milky Way so I do not understand this. It also doesn’t seem to have the same intensity of impact in terms of relaxation. I am trying to pay attention to it more subtly by doing it throughout the day. The jury is out.
Critical Mass RSO: this one is magic. It absolutely relaxes my body. But it can also make me quite high. It is a lovely, floating, tingly, soak into it sort of high. A lie down with your eyes closed feeling every tingle of the body type of high. It is very helpful with sleep, but too drowsy making for daytime use.
The other thing I’m aware of in writing this post is how difficult it is to express the internal feeling of the body in a way others can understand. Each walking video I provide from month to month likely looks exactly like the other to an observer. But the feelings in my legs, in my knees, in my hips can be wildly different, hour to hour, day to day. My walking is hard right now. My spasticity is through the roof. The pain in my hips and sacrum are constant. But you can’t see that in a video, and I try hard not to dwell on them.
This is one way recovery can look almost five months in. This is the dark part of the heroine’s journey, the place of challenge and fortitude, slaying dragons and monsters, holding faith, holding on, holding hope.
In summary, my spasticity is very high. It is known and expected. It is likely to quiet down, though it can take time – months to years, and for some never. So, I’m living in that belief that I am of the many who just have need to hold tight to the wheel through the big waves to the restful pool at the end. The brain is a powerful thing and can write the story. I intend to know that I did my best.
Symptoms:

Walking and legs: this is pretty much covered in the writing above. High spasticity, hip pain, lots of experimentation.
Arm function: ugh. All my energy and attention has been focused on what’s going on in my legs and I really don’t have bandwidth to put the spotlight here.
Bladder: I feel like this is getting better. I can go longer between trips to the bathroom. I still feel urgency and some leakage. I see a pelvic floor therapist this week and I’m excited about that. More to come.
Bowel: Mostly continues to be normal. For some reason I don’t understand I’ve had significant bloating last couple of weeks.
NEW SYMPTOM – Hot Flashes: I have been postmenopausal since 2017. I had minimal hot flashes throughout the menopausal process. Lucky me, they are back! It is a known thing that the chemotherapy agent cyclophosphamide impacts hormones and can put women into menopause early. Given that I was already postmenopausal, I didn’t think this would impact me. Well, it did. I’m having more hot flashes than I was during menopause. Fun.
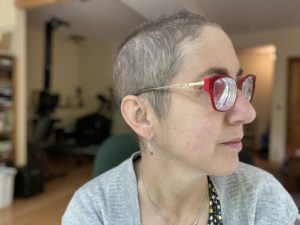
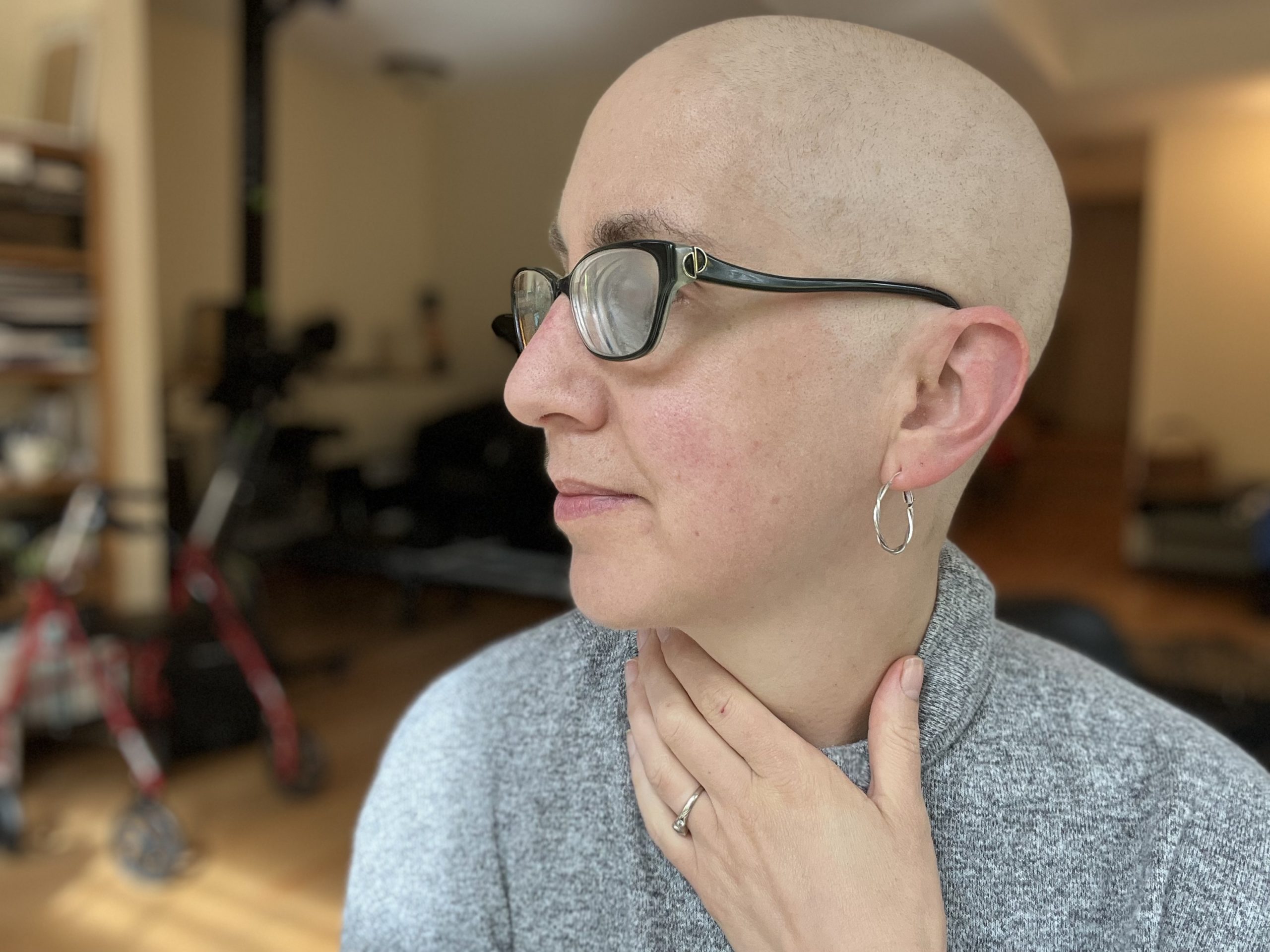
Hair: Hair growth is to the point I no longer look like a cancer survivor. I am fast approaching the decision point of whether to keep at it this length or grow it out. I’ll leave you with that cliffhanger!