Theme of The Month: Spasticity/Spasm Management
Saturday is three months since returning from Mexico. My experience of time passing is both slow and sudden. I cannot believe it has already been three months and at the same time every day feels long and drawn out. It reminds me of how I felt the first year with a newborn.
I have been putting off writing this post because I’ve been struggling a lot in my body. Depending on when I sit down to write, I seem to be either morose and hopeless or excited and hopeful. Today feels more balanced leaning a little towards excited and hopeful. I have had days that feel so hard it breaks me and I sob. I’ve had days where I’ve written in my journal, “this was a fucking good day!” Big swings. This is a boot camp training in Buddhist nonattachment.
I am writing mostly to document the HSCT process and to be able to see changes over time. For that to be useful, I need to be honest and objective about my experience when it is my nature to write an optimistic, future forward, triumphant version of my experience. Well, the last couple of weeks have sucked. My spasticity is still rough. Often, I have periods of spasms so intense and painful that I can’t think of or do anything else.
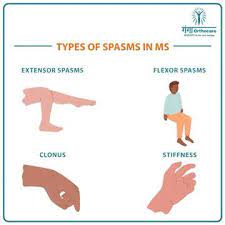
Typically, in the morning, my right leg wants to go into “extensor spasms” where my leg muscles all push simultaneously to extended/straighten my leg as far as it possibly can and with immense force. This hurts. It makes muscle fibers burn and I can’t get it to stop. On the flipside, in the evening, my right leg goes into “flexor spasms” where the entire leg from hip, to knee, to ankle) flex upward suddenly and fiercely, like regimented marching, over and over. This also hurts and makes it next to impossible to do or be anything else.
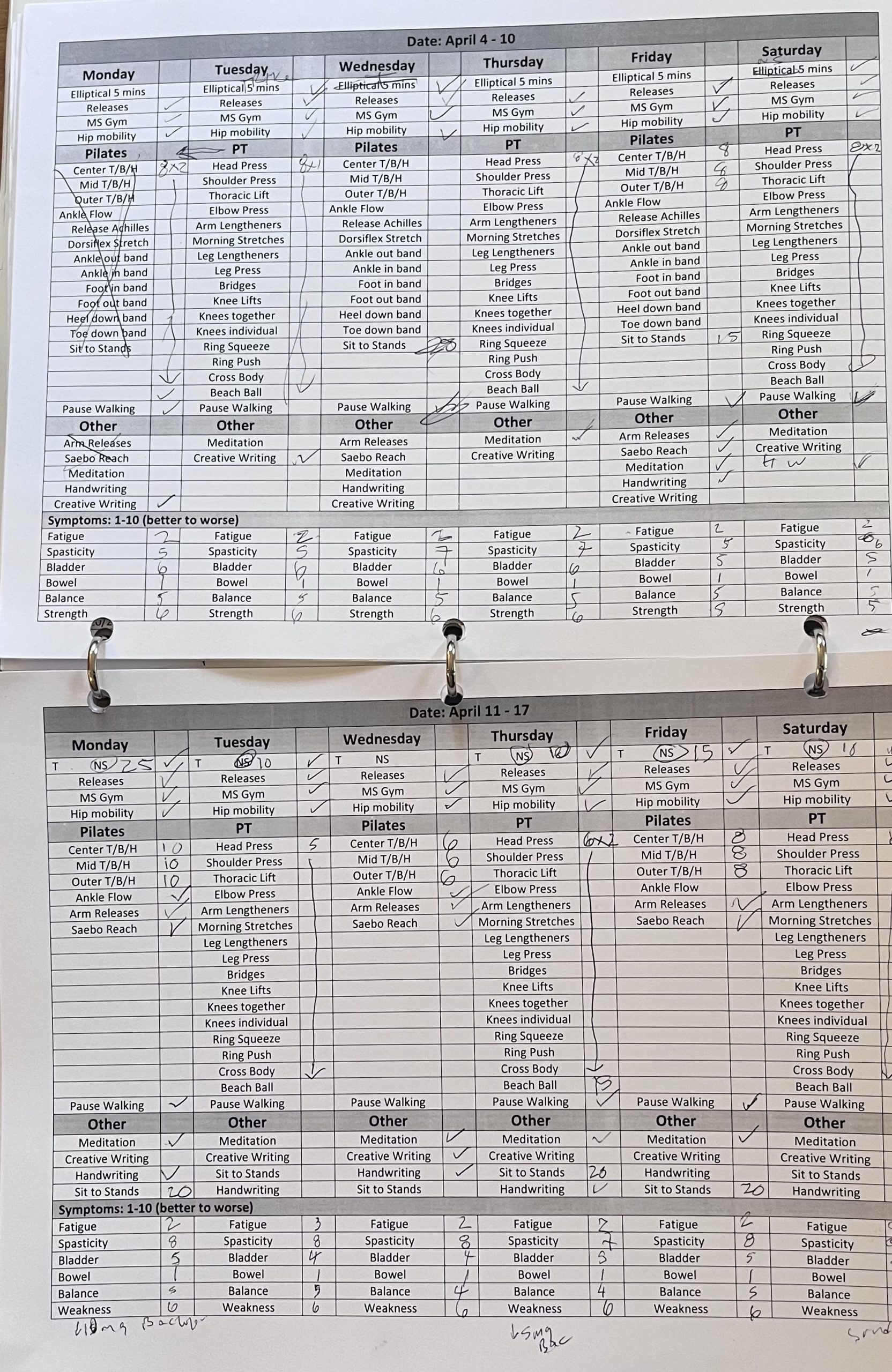
I continue to experiment with different strains, delivery methods, and dosing of different cannabis products. I’ve added more use of ibuprofen, a topical cannabis salve that is remarkable for pain, and topical Voltaren – also for pain. Sometimes I feel like I got it dialed in and then I’ll try the same combination that it won’t work at all. I keep a daily log on my phone to try and find patterns.

“If I take ibuprofen and half a gummy at 5 AM in the morning, does it make it easier to get out of bed?”
“If I make sure to dose with cannabis every two and half hours, do I stay ahead of the spasticity train?”
“Is ibuprofen and topical pain relief more effective?”
“Does it work better if the cannabis is high CBG? High CBD? High THC? Half-and-half?”
It would probably be faster learning if I did this more scientifically, but I want to feel better fast, so I tend to throw things at it with well documented desperation.

I recently ordered a book on managing MS symptoms and found a passage in the spasticity section that outlines “paroxysmal spasms” and describes exactly what I’m feeling. The physician author recommends an anticonvulsant medication, Tergretol. I met with my physician this morning and she has prescribed a similar medication for me, Oxcarbezine, to see if it makes a difference. In her experience this medication is equally as effective with less side effects. I will pick up this prescription this afternoon and get started. It can take up to two weeks to know if it is effective at all and if we need to do any dose changes before determining. Fingers crossed.

Thought process on spasticity causes/triggers:
- MS causes spasticity and I had it prior to treatment. Experience then was of a constant moderate stiffness and difficulty bending ankle, knee, hip on right side. That was pretreatment baseline.
- Increased spasticity, often lasting 6 to 12 months or longer, is common after chemotherapy with cyclophosphamide. Typically people report it starting closer to 8 or 10 months post treatment, but a meaningful contingent have it kick in around 2-3 months post treatment. Maybe I’m in that bucket and that’s why the intensity has increased.
- Decreasing baclofen can cause rebound spasticity. It is unclear how that process is impacting my experience.
- The last couple of weeks have been getting ready to travel to Colorado for Kara’s college graduation. This is a big deal for me three months post treatment. I’m still definitely in recovery and this will take a lot for my body. But it means so much to me to be there that it’s worth it. Is the stress about future events triggering my body to have more spasticity?
- Pain in the muscles of my hips and low back, both caused by spasticity and triggers spasticity. This is why pain management is an important part of this picture.
Two important insights/learnings from the last couple of weeks:
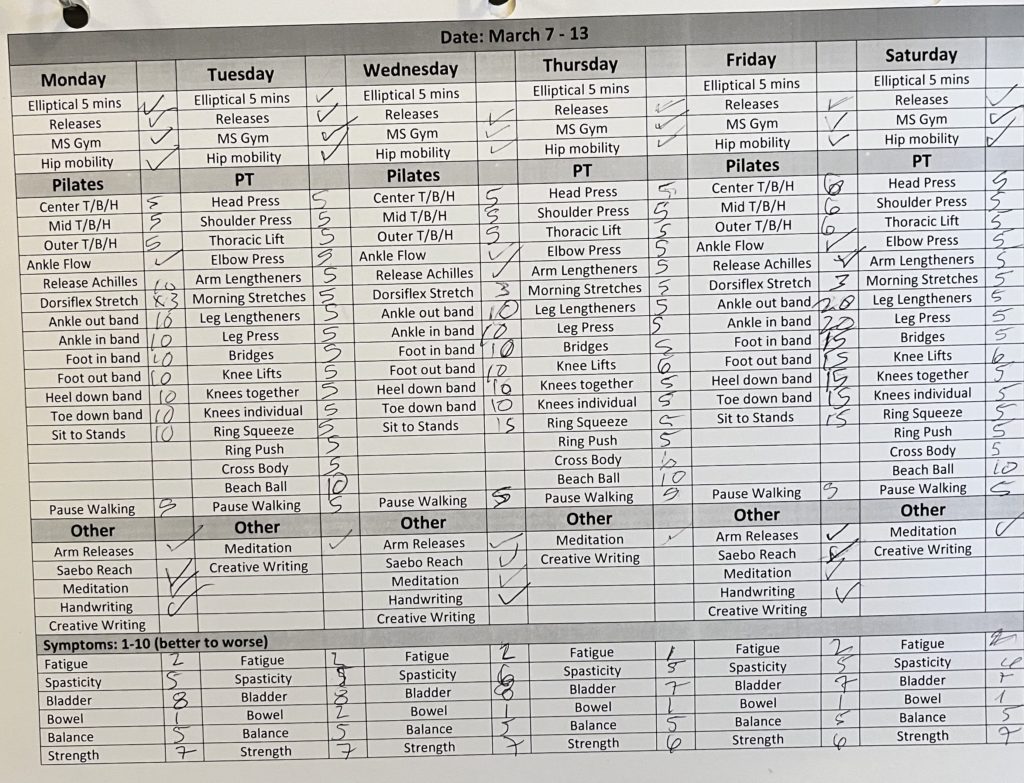
- More is not better. Because of my personality my instinct has been to try and do as many reps of PT exercises as I can and to increase what I can do every couple of days; ultimately to “push”. The more I can do, the faster I will heal right? This is paradoxically untrue. The harder I push, the more my body fights back. I’ve been learning this lesson the hard way. I have made it my practice starting last week to be gentler and to let my body go through the long process of healing. And it is a long game.
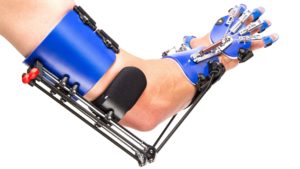
- I have had an AFO (ankle-foot orthosis) for a few years, but barely used it. The device holds my foot in a flexed position (or at least 90° to my shin) and I was nervous that this would increase compensatory movement or cause my ankle muscles to weaken. I started using it over the last couple of weeks and I noticed that it decreases my spasticity and increases stability. For lack of a better description, it makes my brain feel safe and so it makes movement more natural. I have now learned that when I take it off, regardless of what I’m doing, the spasticity can kick in hard, like it was just waiting to spring. My best understanding of this phenomenon is that my brain no longer feels safe when it comes off and it goes into a protective mode. I wait until bedtime, right when climbing into bed, to take it off or the spasticity goes through the roof.

This product is amazing!
Key Moments:
- Baclofen currently at 10 mg per day (5mg AM and 5mg PM). Will decrease the last 10 mg after returning from care’s graduation.
- Met with my PCP on Monday and have begun decreasing tramadol (used for lower back and hip pain for sleep at night). Cannabis “wonder rub” is working wonders, no pun intended. This taper will take approximately six weeks, this is week one.
- 5/17 I clearly felt sensations in my feet that I haven’t felt in a while. Peripheral neuropathy has made the mostly numb, but yesterday they felt more normal like I could feel blood flow through them and I could feel toes move individually. Felt very energetically different.
- Also 5/17 had one of my most difficult mornings where I didn’t know how I would get out of bed and get dressed. The spasming was so painful that I just sobbed. I called mom and she came right over. By the time she got here some of my medications had kicked in, or my body had just come online or something else happened, but I became able to move more freely and find equilibrium again.
- I have tried acupuncture twice over the last two weeks and it has been an uncomfortable experience. My spasticity is so trigger-happy that the needles and the energy created by the acupuncture, whatever’s going on there, explodes the spasticity. Need to keep thinking if this is a helpful path forward.








































 For my own memory and for anyone else’s interest, I wanted to recount the four weekend monumental days that proceeded where I am now. All of this is written in a somewhat fatigue and chemo haze, so again mostly clinical not so poetic.
For my own memory and for anyone else’s interest, I wanted to recount the four weekend monumental days that proceeded where I am now. All of this is written in a somewhat fatigue and chemo haze, so again mostly clinical not so poetic.